Empowering Mobility: Building an Industry-First Connected Device for Prosthetic Limbs
At the AT&T Foundry, our success is dependent upon our ability to move.
Literally.
Our limbs serve as a bridge between our customers’ ideas and deployable products. Our hands construct, modify and refine the prototypes we create. Our arms and legs test these devices in real-world scenarios. Take them away, and it would be much harder for us to do what we do best – innovate.
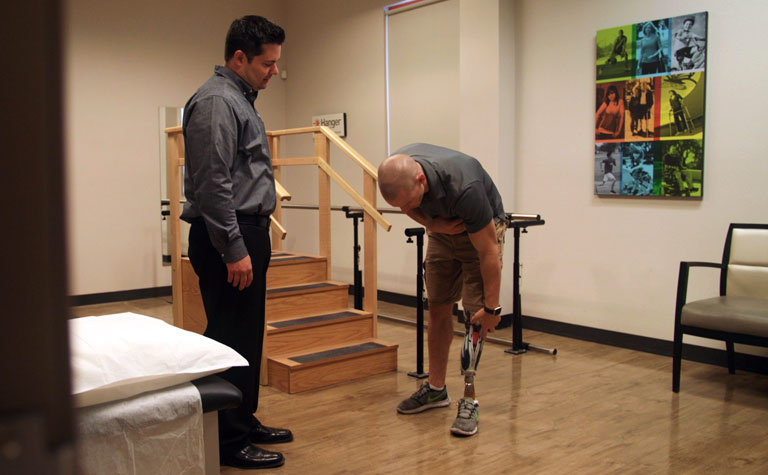
But that’s the reality those living with limb loss or limb difference face each day. For some, adjusting to life with a prosthesis can prove challenging. So Hanger, Inc. came to the AT&T Foundry for help in creating a digital healthcare solution to better reach and serve these patients.
From start to finish, we worked side-by-side with Hanger and its patient care subsidiary Hanger Clinic to ideate, innovate, modify, and ultimately produce a working solution aimed at empowering Hanger Clinic patients to get back to doing what they do best.
Mohamed Mohamed, a biomedical engineer at the AT&T Foundry in Houston, takes us behind the scenes of how we created the prototype for the industry’s first LTE-M, network-connected device for prosthetic limbs.
First of all, what was the challenge driving Hanger’s collaboration with the Foundry?
Hanger is the leading provider of orthotic and prosthetic patient services and solutions, and excels at not only restoring patients’ mobility, but also pushing them to reach for and accomplish their goals. The ability for Hanger Clinic to see how their patients are progressing is currently limited to the clinical setting. Hanger wanted a way to better assist their patients in near-real time so they could make informed decisions on improving the patient experience more quickly. That said, they also have some patients who, for various reasons, may go home and rarely wear their prostheses. Much of our work with Hanger is focused on improving visibility and communication with their patients. That way they could help those patients not just get back on their feet, but also get them back to moving, working and enjoying life faster than they could before. And for Hanger to reach those patients faster, we needed to move fast as well.
What did you create for Hanger?
Hanger’s goal was to test the feasibility of a prosthesis with integrated network connectivity – one that could send Hanger useful data on various patient metrics on prosthetic usage.
We created a small, separate device that mounts directly onto below-the-knee prostheses. To give Hanger a complete picture of the patient experience, we fit that device with an LTE-M modem and 3 sensors that collect data on various ranges of motion and directionality. An accelerometer captures speed of motion and force of impact. A gyroscope monitors how the device swings and tilts in space. A magnetometer sends information about direction and heading, much like a compass.
Combined, these sensors allow Hanger to discern type of motion conducted, such as whether the patient is walking, running, or going up or down stairs. It also reports on how often a patient is active, how long and the degree of activity per event.
By providing Hanger with a custom activity tracker, we paved the way for them to develop and implement more sophisticated motion tracking algorithms. So in addition to gathering a richer understanding of patient activity, Hanger can view their patients’ walking patterns and stability. This may help reveal when a prosthesis might be reaching end of life or needs to be adjusted to fix issues affecting a patient's gait. And that’s especially important for first-time prosthetic users who are still adjusting and might be dissuaded from using their prostheses by initial, unknown challenges.
To tie all this data together, we created a prototype for an interactive, iOS mobile app that lets patients do things like track their progress or contact Hanger Clinic for support. Likewise, Hanger Clinic clinicians can view their patients’ dashboards and reach out to those who appear to have an issue with their prostheses.
What was the innovation process like?
Like all Foundry projects, the path to a finished prototype wasn’t a straight line. Ensuring we created an intuitive prototype that could fit easily into patients’ everyday lives required various trials and close collaboration.
Making sure the device can be used on most below-the-knee prostheses that Hanger Clinic creates was an interesting challenge. Every prosthesis Hanger Clinic designs and fabricates is unique to each individual patient. That means there are a lot of variables when it comes to the mechanical components and their dimensions. Thanks to rapid prototyping technologies such as 3D printing, we were able to quickly make iterations on the physical design of the device and see how it fits onto various forms of a prosthesis.
Did you experience any major challenges? What helped you overcome them?
Absolutely. At the Foundry, we like to treat innovation as a contact sport, and that was certainly the case while creating this device.
Our initial prototype was larger than ideal for real-world use. But this not-so-beautiful, bulky version allowed us to have something in hand quicker to test out the software for capturing the metrics Hanger wanted, and to begin looking at the data. While improving on that element, we were able to work in parallel to design and build a custom device that was more compact and easier on the eyes. Working together in this nimble group and being able to reach out to other engineers in the Foundry family allowed us to make the fixes we needed to move forward. And with every step closer we were learning something new.
Expediting this entire process was the convenience of having a Hanger Fabrication Lab and a local Hanger Clinic location within 5 miles of the Foundry in Houston. We spent many hours with Hanger Clinic in their lab modifying the device fit and alignment on the prosthesis. We even tested the device with a few of the Hanger Clinic employees who use the same prostheses this device will serve.
What was the key driver in creating a successful prototype?
What keeps innovation moving forward is continued motivation from collaborators and a clearly defined vision. It was inspiring to have that direct experience with the end users at Hanger Clinic testing the device. And seeing the various iterations of the device ignited my drive for this project and maintained my clarity of vision for what the device hopes to accomplish – empowering human potential.

Mohamed joined AT&T in March 2016. He graduated from the University of Houston with a PhD in Biomedical Engineering.

Vishy Gopalakrishnan – Vice President, Ecosystem & Innovation
.jpg)